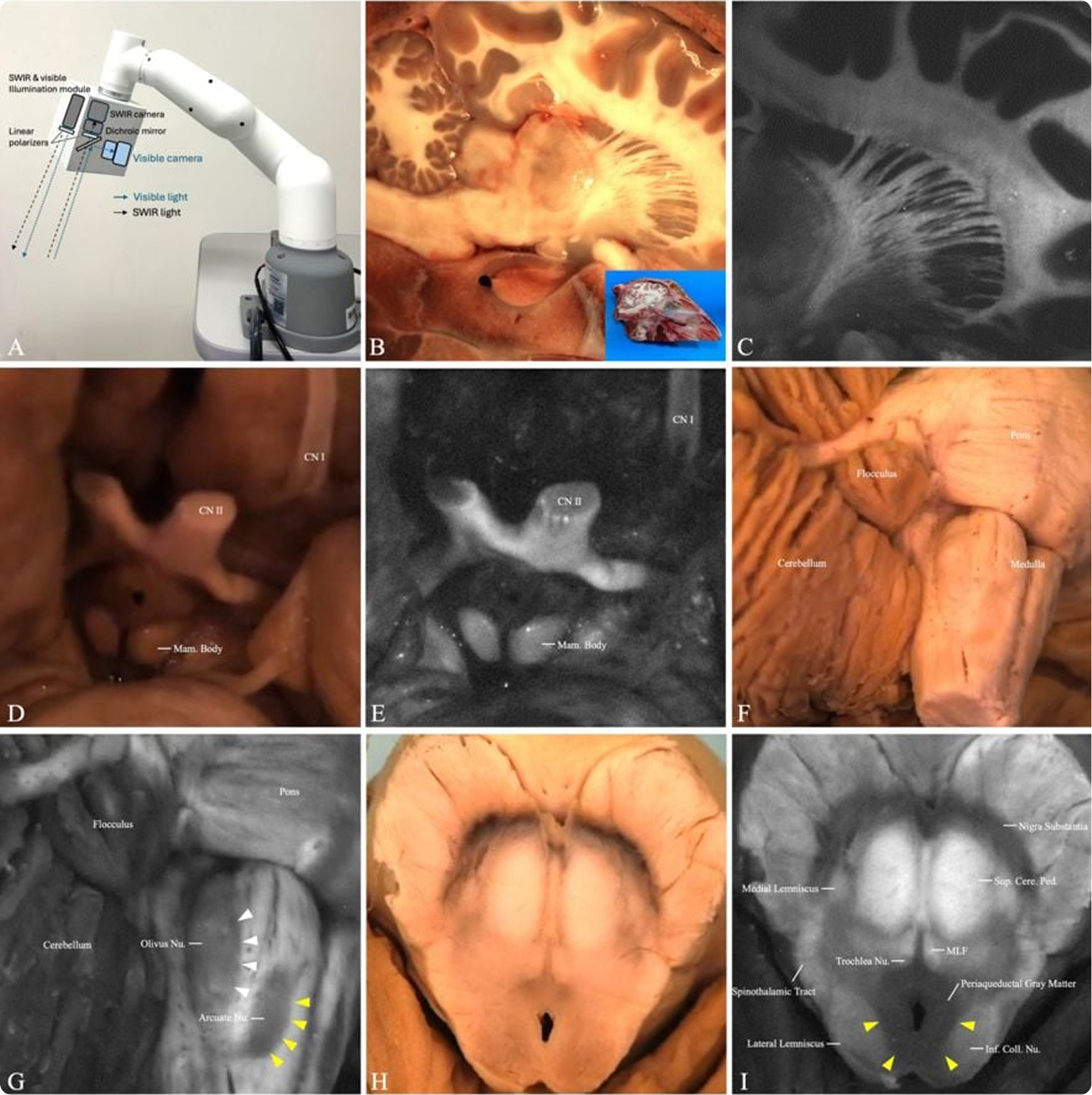
Abstract
Lymph node dissection is an important step in grossing, in which findings go on to affect patient prognosis and care management. The standard technique for finding lymph nodes is through manual palpation – an expertise that usually takes years to gain. The only way to improve on such skills is through practicing through the real clinical cases, where patient care is on the line. This could present potential possibilities for less-than-optimal patient outcomes. Fixatives, such as Dissect Aid and Carnoy’s solutions, are sometimes used to help address this issue. But they significantly increase the overall turnaround time, expose prosectors to potential health hazards, while still only marginally mitigate the issue. In this abstract, we introduce the InVision, a new optical imager for gross examination produced by Cision Vision, as a new modality that will aid finding lymph nodes and gaining experience for newer and inexperienced prosectors, without sacrificing patient care. Its real-time imaging capability also removes the need for chemical fixative – shortening the turnaround time and eliminating exposure to health hazard.
Background
Lymph node status and yield are major indicators in prognostication and cancer care management. The N-stage and number of metastatic lymph nodes yielded during grossing go on to define patient treatment and suggest patient prognosis. Although there are lymph node minimums in certain tumor types, literature1 suggests that finding lymph nodes in excess of these minimums provides higher quality patient care. Generally speaking, a higher yield of lymph nodes provides more confident insight to lymph node staging and thus avoiding understaging and its consequence of withholding vital treatment for the patient.
Literature2 suggests that inconsistencies in lymph node yields can be found at the hospital level. Prosectors of lymph node dissection range from pathologists, Pathologists’ Assistant, or the residents. Gaining expertise and skill in the difficult craft of lymph node searches through manual palpation requires practice in caseloads. This means that inexperienced prosectors must begin their practice on real patient specimens.
While the learning-through-doing approach is generally true for medical practitioners throughout different specialties and tasks, lymph node searches through manual palpation is unique in three different aspects – (1) it is extremely clinically consequential, (2) it is extremely technically challenging, and (3) mistakes are not detectable due to intrinsic variabilities across individual specimens.
While there is not a defined expectation of efficiency for newer prosectors, time is a valuable and finite resource, especially since most gross rooms are severely understaffed. The time pressure to fulfill considerate amount of workload responsibilities while gaining experience at the same time means patient care can potentially be comprised along the way.
Current alternatives exist but are limited to chemical aids, of which available options are limited to irritants and carcinogens, and all require additional fixation. Non-chemical aids currently do not exist as a standard of care.
InVision is based on a new optical imaging modality invented by Cision Vision. It uses ex-military technologies that were previously inaccessible to civil applications. The fundamental mechanism is that InVision uses shortwave infrared light that lets the natural water content contrast between fat and lymph nodes manifest itself in real time without any injection or radiation. Most importantly, it does not replace the manual palpation, but rather enhance it by providing an additional dimension of information – real time visual feedback. In the context of prosector education, the tactile feeling memory of lymph nodes through manual palpation can be reinforced by the visual feedback – therefore potentially shortening the learning curve for gaining expertise in lymph node searches.
Methodology
The prosectors begin lymph node dissection by sectioning and removing fat or other soft tissue with suspected lymph node candidates, and place against the screen of the device. With the tissue of interest on the functional platform, the prosector manually palpates for lymph nodes, and/or sections the tissue to reveal lymph node candidates. While the prosector grosses for lymph nodes against the platform, the device screen reveals a contrasted image that highlights lymphoid tissue against non-lymphoid tissue. Lymphoid tissue appears as a darker structure, while fatty tissue appears as lighter-to-translucent structures. The prosector combines the manual palpation and/or sectioning with the visual contrast provided by the device to more quickly acknowledge and submit lymph nodes for histopathology.
As a proof-of-concept study, subjective interviews were carried out to assess the usability and the potential educational value of the InVision product. Users with different experienced levels, from PA students, residents, pathologists and extremely experienced PAs, were interviewed and surveyed.
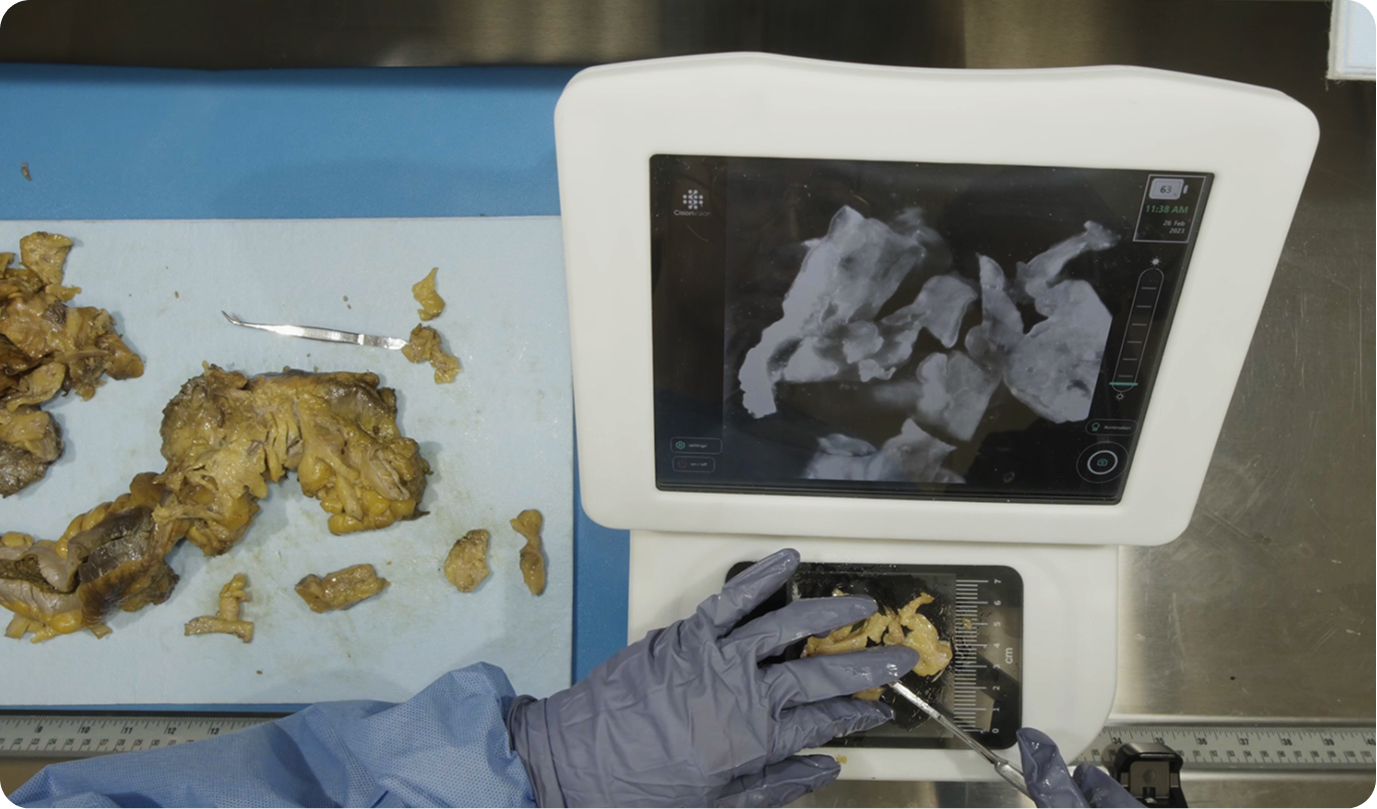
InVision’s workflow in a grossing bench
Results
The interviewees expressed unanimous positive responses to the usability of the InVision product. Quotes include:
“That’s amazing. The amount of Friday nights in residency that could have been save by this are ridiculous” – Pathologist.
“I love this idea — something that we had been dreaming of as residents.” – Pathologist
“I became a neuropathologist because there wasn’t something like this when I was a resident years ago.” – Pathologist
“This device definitely makes finding lymph nodes a lot easier and it gives you the confidence that there is no lymph node left in the residual fat tissue even after the first round of gross.” – Resident
“This definitely helped me find lymph nodes that I could have missed.” – PA with 20+ years of grossing experience
“This makes finding lymph nodes far less intimidating. It also makes the process far less tedious too.” – new PA with minimal experience
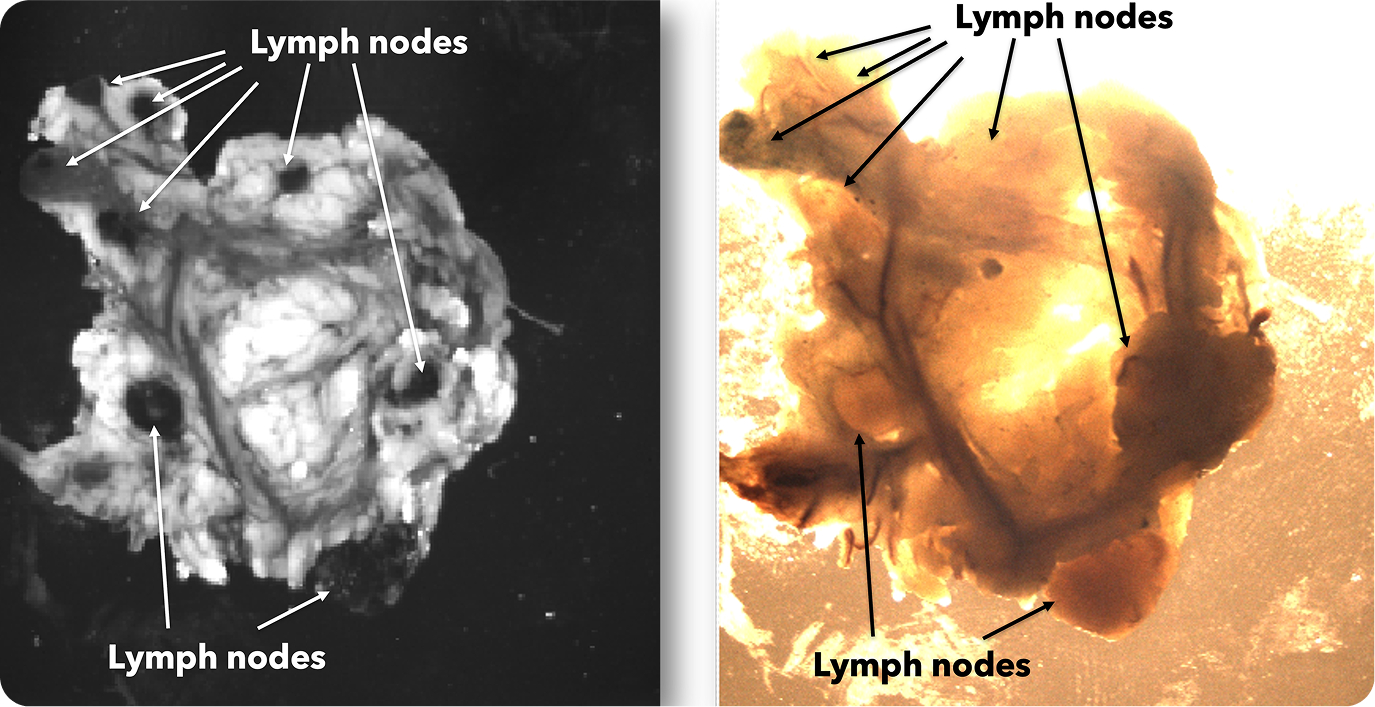
Lymph node network in the mesentery specimen
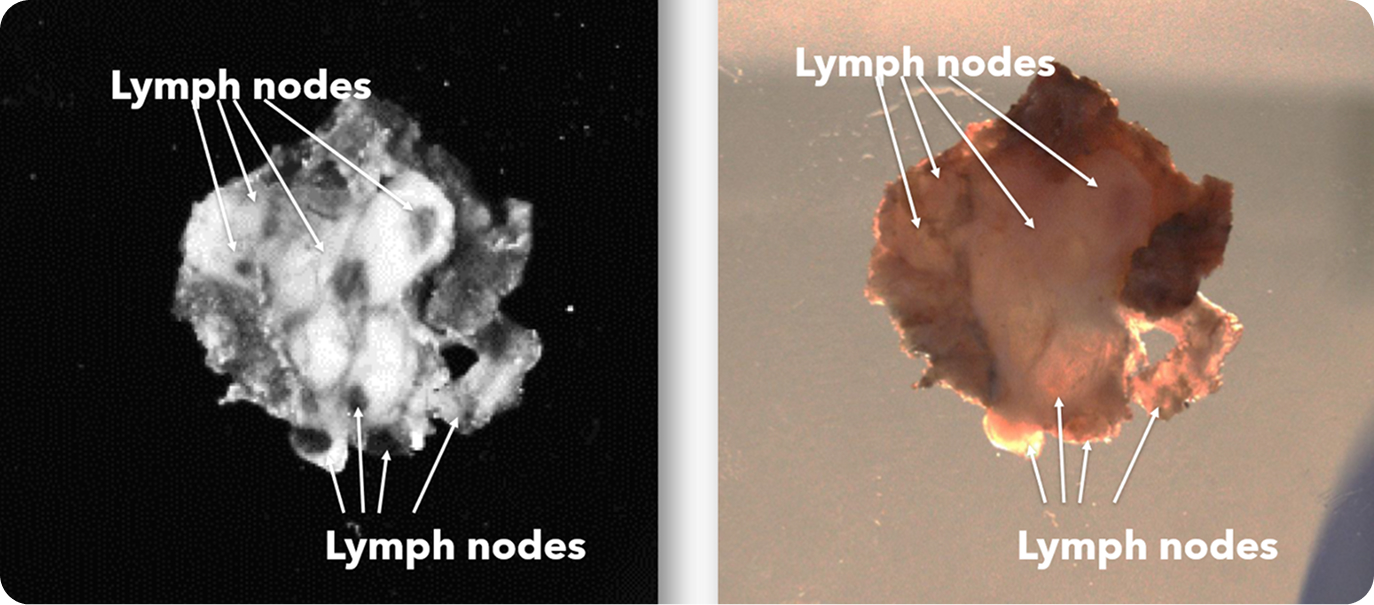
Lymph node network in head and neck specimen
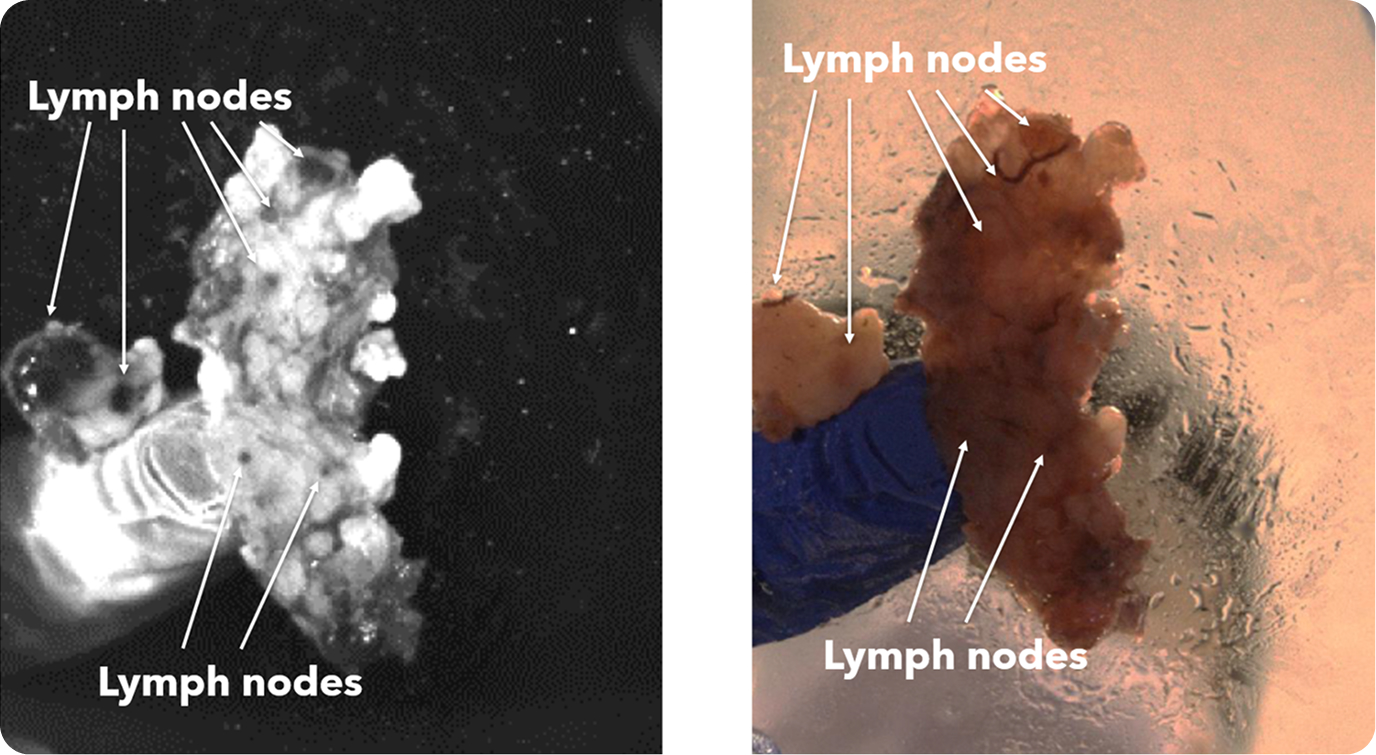
Large and minute lymph nodes in head and neck specimen
Conclusion:
Lymph node yield is paramount to patient care and prognosis, and may be affected in a learning setting with newer prosectors. The InVision device introduces a new modality to lymph node dissection and can be a valuable tool in reinforcing confidence and experience, without sacrificing patient care.
Authors
Cision Vision
Mountain View, CA
Cision Vision
Mountain View, CA