
Summarized by
Matthew Rosenbaum, MD
Beth Israel Deaconess Medical Center
Harvard School of Medicine
Background
The total number of lymph nodes examined during colorectal cancer (CRC) resection is often considered a quality metric. However, the number of negative lymph nodes (NLNs)—has emerged as a potential independent prognostic factor. This study aimed to determine whether NLN count predicts survival.
Methods
This analysis included 716 non-neoadjuvant CRC patients (stages I–IV) from the Nurses’ Health Study and Health Professionals Follow-Up Study cohorts. Molecular features assessed included microsatellite instability (MSI), CpG island methylator phenotype (CIMP), KRAS/BRAF mutations, p53 expression, LINE-1 methylation, and lymphocytic immune response. Patients were grouped by NLN count (0–3, 4–6, 7–12, ≥13), and outcomes were assessed using multivariate Cox proportional hazards models.
Key Findings:
A mean of 11.9 total lymph nodes were found (median:10, 25th %ile:6, 75th %tile: 15, range 0–55, highlighting a high degree of variability and general difficulty getting the prerequisite number of lymph nodes.
- Survival Association:
Higher NLN counts were significantly associated with improved overall and CRC-specific survival (p < 0.0001), even after adjusting for tumor stage, molecular markers, immune response, and a myriad of other clinical factors. Multivariate HR for all cause mortality was 0.46 in patients with greater than 13 LNs compared to those with 0-3 LNs.
- Stage-Specific Effect:
The survival benefit of increased NLNs was observed across all stages but was more pronounced in stages I–II than in stages III–IV (interaction p = 0.002).
- No Plateau Effect:
Spline analysis revealed no threshold beyond which additional NLNs ceased to confer survival benefit.
- Lymph Node Ratio (LNR):
Among stage III–IV patients, a lower LNR (lyph node ratio: positive/total nodes) also independently predicted better survival.
- Independent of Molecular Features:
The prognostic value of NLN count was independent of MSI, CIMP, BRAF, and LINE-1 methylation status, as well as lymphocytic inflammation.
- Study limitations:
Most CRC were diagnosed in the 1980s-1990s when the grossing standard was not as rigorous than it is today, although this gives us a real-world situation demonstrating the important of proper grossing in prognostication. Also not all data or tumors were able to be retrieved and analyzed but this did not appear to bias the data set.
Key Outcomes by Negative Lymph Node Count
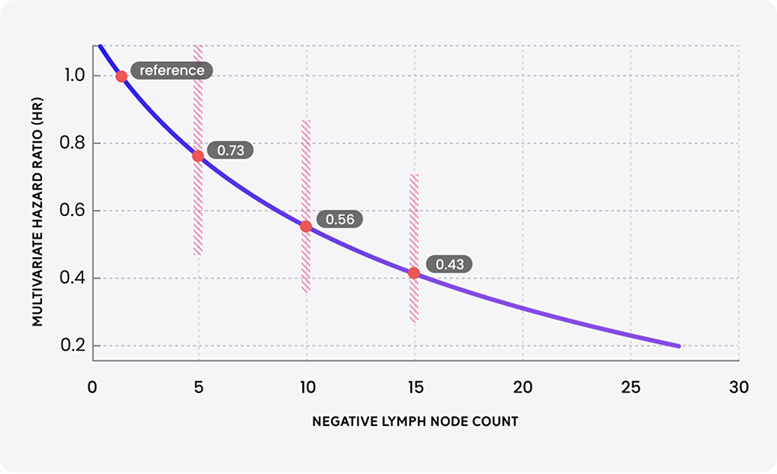
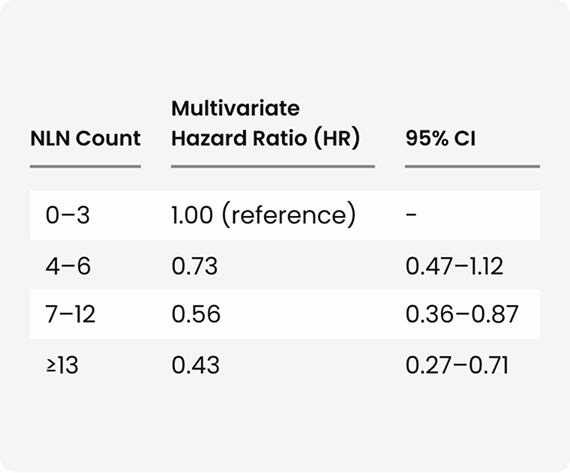
Conclusion:
Negative lymph node count is a robust, independent prognostic factor for colorectal cancer survival. It remains significant after adjusting for known molecular, immune, and clinical predictors and may reflect tumor biology, host immune competence, surgical quality, or a combination of these.